Table of Contents
ToggleLosing a tooth changes more than the way a smile looks. It can make chewing less comfortable, leave a gap that traps food, and over time it can affect the bone and teeth around it. That’s why dental implants come up so often when people start looking at long-term options for replacing missing teeth. They’re designed to take over the job of the missing tooth root, not just fill the visible space above the gums.
What is a dental implant, exactly?
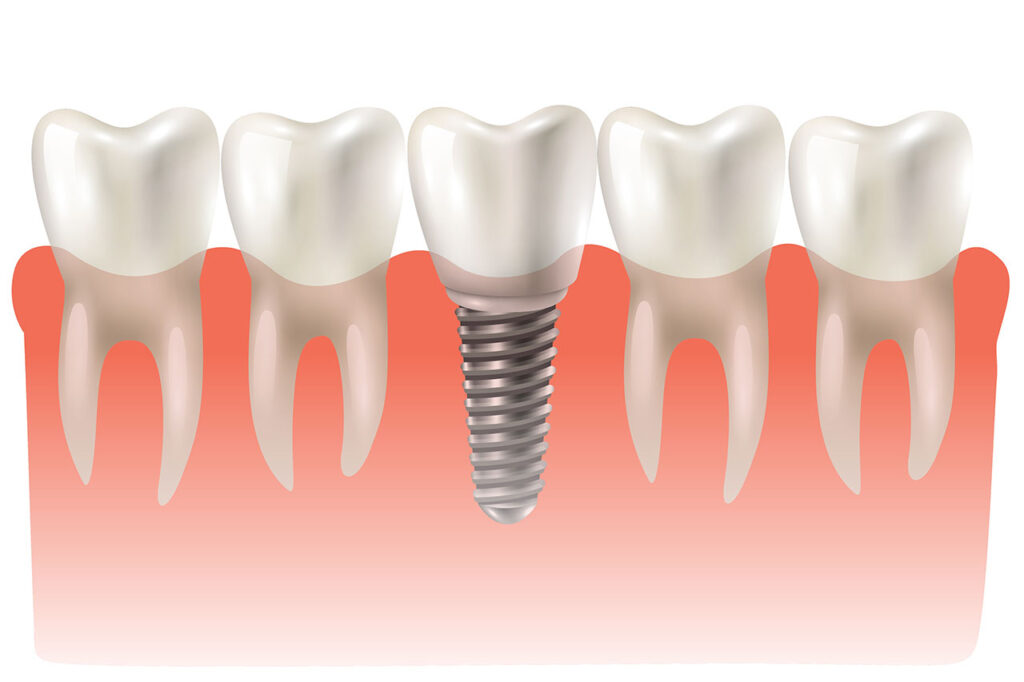
A dental implant is a small metal post, usually made from titanium, that is placed into the jawbone where the missing tooth used to be. Once it heals, it acts like an artificial tooth root. A custom-made replacement tooth is then attached to it, so the final result looks and functions much more like a natural tooth than a removable option. Australian oral health sources describe it in plain terms: the implant sits in the bone, and the new tooth sits on top.
This is the key difference between implants and some other tooth replacement options. A denture mainly rests on the gums. A bridge fills the gap by relying on neighbouring teeth for support. An implant goes into the jaw itself, which is why it can feel more secure once treatment is complete. It also means the healthy teeth next door often don’t need to be cut down just to support the replacement.
How do dental implants replace missing teeth?
The process works in stages. First, the implant post is placed into the jawbone. Then the bone heals around it and locks it in place. You may hear dentists call this “osseointegration”, but the simpler version is that the bone and implant join together closely enough for the implant to act as a stable anchor.
Once that healing stage is complete, the visible replacement tooth is attached. If one tooth is missing, that’s usually a crown. If several teeth are missing, implants can support a bridge. If all teeth in one jaw are missing, implants can also help hold a full denture in place. So although many people think of implants as a single-tooth fix, they can also be used in wider restorations.
Why the jawbone matters so much
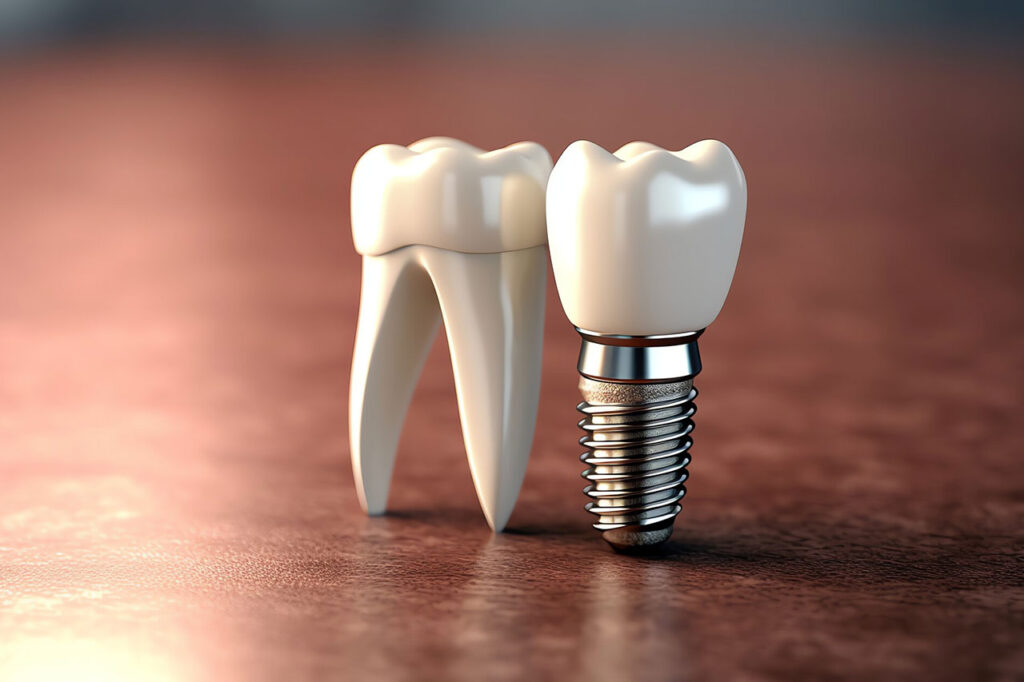
A natural tooth root does a quiet but useful job every day: it transfers chewing forces into the jawbone. That stimulation helps maintain the bone in the area. When a tooth is removed and not replaced, the bone can start to shrink over time. That’s one reason missing teeth can lead to more than a cosmetic problem. It can affect bite stability and, in some cases, the position of nearby teeth.
Because implants rely on bone for support, bone quality matters. Your dentist will usually check the site with dental imaging, often including a 3D scan, to see whether there is enough bone to hold the implant safely. If there isn’t, extra planning may be needed. Some patients need bone grafting before or during implant treatment so the implant has a stronger foundation.
What does the dental implant procedure usually involve?
Treatment normally starts with an assessment rather than surgery. The dentist checks the gums, the bite, the amount of available bone, and your general health history. More than one appointment is usually needed to plan and complete implant treatment properly. That staged approach helps reduce surprises later.
The surgical appointment places the implant into the bone. After that, there is a healing period before the final crown, bridge, or denture is connected. Some clinics offer immediate or faster-loading options for selected cases, but many standard implant treatments still take several months overall. Exact timing depends on healing, bone levels, whether an extraction was needed, and whether bone grafting is part of the plan.
Are dental implants right for everyone?
Not always. Many adults are suitable candidates, but implants are not automatic for every missing tooth. Dentists look closely at bone volume, gum health, smoking status, and medical history. Experts note that severe gum disease and smoking can reduce suitability, and some health conditions or medicines can also affect planning.
That doesn’t mean implants are off the table the moment a problem appears. It often means the case needs more preparation. A person may need gum treatment first, better plaque control, smoking reduction, or extra imaging and grafting. Good implant treatment is rarely about speed alone. It’s about whether the site is healthy enough to support a stable result.
What are the benefits, and what should people keep in mind?
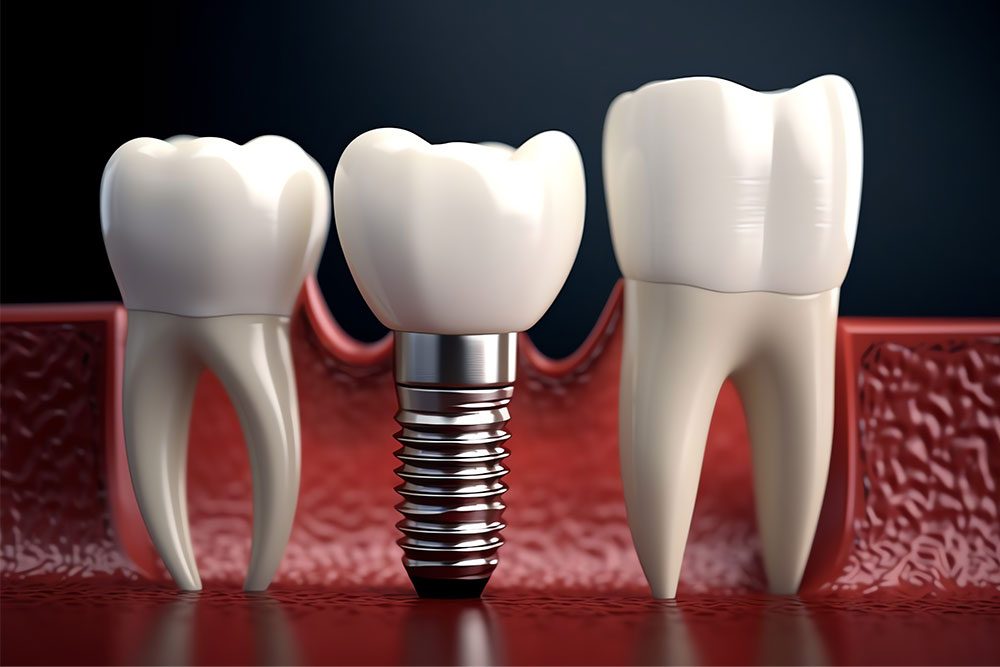
For many patients, the appeal is straightforward. Implants can look natural, feel stable, and let people chew more normally than they can with a loose replacement. Implant treatment usually does not involve the neighbouring teeth in the way some bridge treatment does. That can be a real advantage when the teeth beside the gap are healthy.
Still, implants are a surgical treatment, so they come with real risks and responsibilities. Healthdirect lists possible complications such as infection, nerve damage, sinus problems, and injury to surrounding teeth. There is also a small risk that an implant may not integrate properly with the bone. On the positive side, long-term outcomes are strong when cases are planned well and maintained properly, with systematic reviews reporting high survival rates for single implants over time.
How do you care for a dental implant?
An implant isn’t “fit and forget”. It needs daily care, just like natural teeth. The implant itself cannot get tooth decay, but the gums and bone around it can still become inflamed. If plaque builds up and that inflammation is ignored, peri-implantitis can develop, and that can threaten the stability of the implant.
The basics are simple: brush twice a day, clean between the implant and nearby teeth every day, and keep up with regular dental check-ups and professional cleans. Australian Dental Association guidance also notes that floss, interdental brushes, or a water flosser may be used depending on the type of implant restoration and the spaces around it.
Dental implants are popular for a reason. They replace the missing root as well as the missing tooth, which gives them a more stable, bone-supported role in the mouth. They aren’t the right answer for every person or every gap, but when the case is suitable and the aftercare is solid, they can be a durable way to restore function and confidence.